Health
Revolutionary Deep Brain Stimulation Offers Hope for Parkinson’s Patients
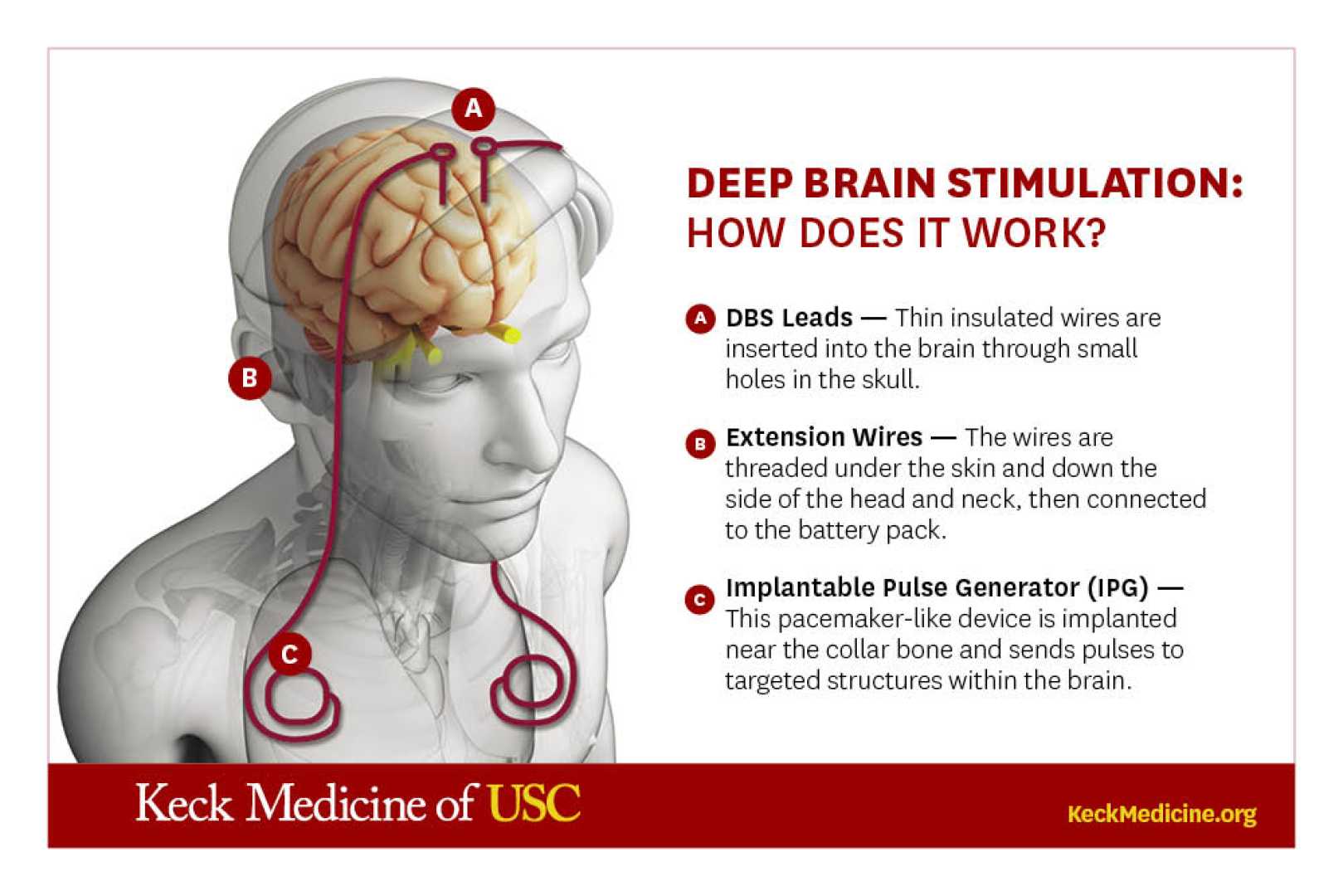
Boston, MA – Researchers are making significant strides in treating Parkinson’s disease through a novel approach to deep brain stimulation. A study by Busch et al., published in npj Parkinson’s Disease, reveals that chronic adaptive deep brain stimulation (aDBS) holds great promise for improving patient outcomes.
Parkinson’s disease affects millions globally, causing severe motor symptoms like tremors and rigidity. Traditional deep brain stimulation (DBS) provides continuous electrical pulses to specific brain areas but does not adjust to the fluctuating nature of neurological symptoms. This new aDBS technique uses real-time neural feedback, enabling stimulation levels to adapt according to individual patients’ needs.
The research highlights a comprehensive study involving patients with Parkinson’s disease, wherein the aDBS method resulted in significant enhancements in motor function, particularly in reducing bradykinesia and rigidity. Patients reported fewer tremors during off-medication periods, and this was achieved while decreasing overall stimulation intensity, benefiting both efficiency and safety.’,”
According to the study, precise calibration of DBS parameters is crucial for approximately balancing symptom relief with the preservation of quality of life. The researchers noted a notable improvement in unified Parkinson’s disease rating scale (UPDRS) scores, indicating that aDBS may be a more effective alternative to conventional treatments.
Another critical aspect of aDBS is its programmable flexibility. Unlike traditional methods that often require frequent clinical visits for adjustments, aDBS can automatically modify stimulation levels based on indications from patients’ neural activity, making it a more proactive approach.
The technology behind aDBS is advancing significantly. The research team described novel sensing electrodes and onboard signal processing capabilities that enhance the precision of these devices. These innovations open new avenues for managing Parkinson’s disease more effectively, considering individual patient variability.
While aDBS shows great promise, challenges remain, including the complexity of deploying personalized algorithms for individual patients. Continued research is needed to ensure the reliability and safety of new technologies as they are integrated into clinical settings.
Looking ahead, the team aims to broaden the range of monitorable biomarkers and improve the systems by incorporating wearable technology. This integration could lead to a more comprehensive treatment that addresses not just motor symptoms but also cognitive and mood-related challenges.
This pioneering research underscores the transformative potential of closed-loop neurotechnology in Parkinson’s disease, paving the way for more precise treatment options. As technology and understanding of the disease progress, adaptive DBS might eventually become standard practice, offering hope to many battling Parkinson’s disease.












